
8 February 2024
Below are key facts about the NHS over the last 14 years. Candidates may find this briefing useful for deciding whether to take our Pledge for the NHS and/or formulating their campaign messaging. Activists may find it useful for making the case to candidates to take the Pledge for the NHS.
The Health Secretary's legal duty to provide
Until the passage of the Health and Social Care Act in 2012, the Health Secretary had a legal duty to provide health services, and put in place all the “reasonable requirements” for this, in England. The Health Secretary's duty was repealed by the Act and transferred to regional health bodies.
Because that duty was transferred from the Health Secretary to individual regional NHS bodies (first to the Clinical Commissioning Groups; now the Integrated Care Boards (ICB)), the quality of care patients get now resembles a postcode lottery. It depends on how good a job their regional ICB is doing and on how well they are managing their limited budgets.
Restoring a national duty will mean patients can hold the health secretary accountable for maintaining a standard of service across the country.
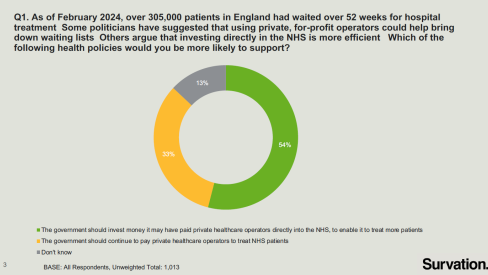
Combined with Section 75 of the 2012 Act, which made it compulsory in most instances to tender out contracts for services, the change of the duty from “providing” to “arranging” has led to the growth of privatisation in the NHS. In the first year of the 2012 Act, one-third of NHS contracts went to private companies.
Our NHS is being systematically underfunded
- According to analysis by Health Foundation, between 2010 and 2019, healthcare spending per head in the UK lagged behind the European average by £40 billion per year. Compared to similar (in terms of GDP and population size) countries like France and Germany, we spent £40 and £73 billion less per year over that period respectively.
- Furthermore, a British Medical Association’s analysis suggests that if NHS funding kept pace with its 4.1% average historical growth rate (1955-2010), the NHS would have received £322 billion more than it received between 2010 and 2022.
- Politicians talk about wanting to modernise the NHS, but the lack of adequate resources is undermining the NHS’s ability to advance a substantive modernisation and digitisation agenda, with NHS managers being forced to make cuts to IT and innovation budgets to ensure underfunding doesn’t hit patients directly.
Why privatisation is bad for patients and the NHS
Profit-seeking makes the NHS less efficient.
Figures on how much profit leaves the NHS from NHS contracts with private companies are difficult to access, because private contracts are by their nature opaque and in many cases, secret. This by itself provides an argument against privatisation.
But we have some indications of how much is leaving the NHS in the form of profits.
- A Financial Times analysis of profits from PFI contracts between 2011 and 2016 (just one form of NHS privatisation) suggests at least £831 million had left the NHS in shareholder profits in that time.
- The Centre for Health in the Public Interest analysis suggests that PFI companies have made £1.9 billion in profits out of the NHS's budget in the last 17 years.
Privatisation causes problems the public has to pay for.
Like in the case of profits, no overarching analysis exists for how much has been spent to fix problems created by NHS privatisation but we have illustrative examples:
- Outsourced cleaning and infections. Academic analysis shows that NHS hospitals cleaned by in-house staff are cleaner and result in fewer hospital-acquired infections than those cleaned by private outsourcing companies. Estimates suggest that there are 300,000 cases of hospital-acquired infection in the NHS yearly, costing the NHS an extra £1 billion each year.
- Private hospitals hand patients to NHS A&E. Another example, revealed by the Sunday Times, is the fact that over 550 people receiving treatment in private hospitals, who develop medical emergencies while there, are then transferred to NHS hospitals every month. This last issue has been cited by Oxford researchers when linking NHS outsourcing to 557 treatable deaths.
Privatisation has driven down overall quality.
Our NHS was ranked number one among the healthcare systems of eleven developed economies compared in terms of efficiency, care quality and overall by a 2014 Commonwealth Fund study. The UK has fallen to fourth place in the 2021 edition of that same study. It is no accident that this decline has coincided with the growth of outsourcing caused by the 2012 Health and Care Act and the systematic underfunding of the NHS over the last 14 years.
Nothing can take the place of proper staffing and building NHS capacity
- The NHS has played a world-leading role in new diagnostic and treatment technologies, in a way that a profit-oriented system simply cannot. We must defend this proud history of adapting and modernising to solve new problems for patients:
- 1960s — advancements in hip replacement surgeries.
- 1987 — the world-first heart, lung and liver transplant in 1987
- 2021 — ran RECOVERY as “the world’s largest trial into treatments for COVID-19, with more than 40,000 participants across 185 trial sites in the UK”
- Investing in modernisation cannot open the door to privatisation and, even more importantly, cannot take the place of proper investment in staff and capacity. This was made clear by a 2018 joint report by the Institute for Fiscal Studies and leading health policy experts. A 2022 analysis of the NHS workforce by The Health Foundation found that the service needed 103,000 more staff than it had in 2021/22 and projected that by 2024/25, that number will have risen to 179,000.













Comments
Dee Harvey replied on Permalink
Keep our NHS free at point of need for all and out of the hands of private profiteers
Heather L Peacock replied on Permalink
I have worked for the NHS for over 30 years. We need immediate action on our amazing institution. The NHS has been run down by the Conservative government so people will go private. The connection between Conservatives and private healthcare are public knowledge. We need to stop the privatisation and out sourcing for proper public healthcare.
Dan Jerrome replied on Permalink
As the Green Party candidate for Stretford and Urmston I will always campaign and argue for our NHS. We're the only national party being honest about the scale of the problem and the funding that is needed.
Jess Lee replied on Permalink
So glad that I represent a party that understands how vital NHS recovery is. As the daughter of a mother who remembers the untold distress in the backlog of untreated health conditions which came to light when the NHS first began, I will always rally to the principles of the NHS and the people who staff it day in day out. The mother of my mother's schoolfriend had lived with a prolapsed womb for at least a decade, and could not afford treatment during the depression and war years. After the NHS came in, this woman's suffering was alleviated and she went from anaemic and poorly, to confident and blooming.
Add new comment